See Prompt in action!
Thank you! Your submission has been received!
Oops! Something went wrong while submitting the form.

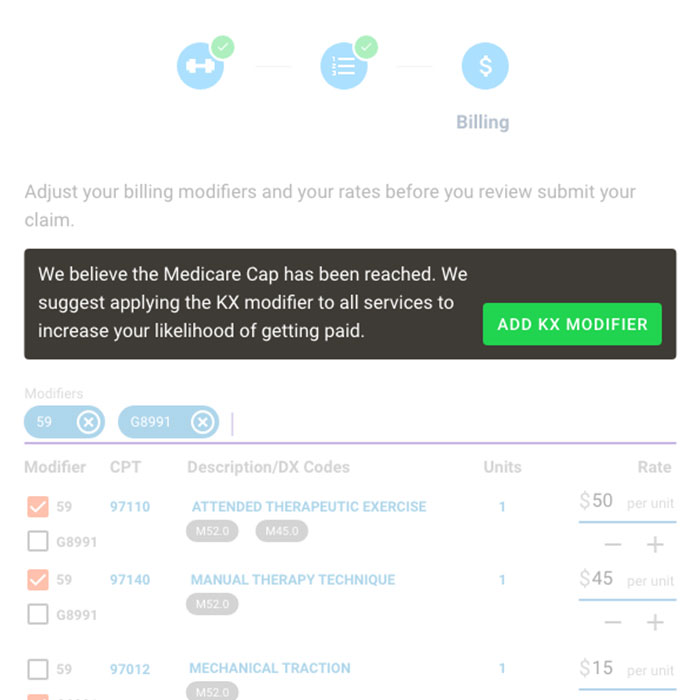
Learn how to optimize your Medicare documentation to ensure you are proving medical necessity and getting the proper reimbursements.
With over 30% of all physical therapy visits involving Medicare, documenting for Medicare is crucial and proving medical necessity is a requirement. We have broken down the Medicare Local Coverage Determination (LCD) for New Jersey to provide you with tips on documentation best practices when dealing with Medicare.
Clause: “Therapy services are considered skilled when they are so inherently complex that they can be safely and effectively performed only by, or under the supervision of, a qualified therapist.”
Key finding: To get paid by Medicare, you must treat the patient with direct supervision from a therapist and document why the patient can’t perform the activity without a therapist present.
Clause: “These skilled services may be necessary to improve the patient’s current condition, to maintain the patient’s current condition, or to prevent or slow further deterioration of the patient’s condition.”
Key finding: You must document how the services you are providing are improving, maintaining, or preventing deterioration of the patient’s condition.
Medicare will cover services provided to maintain the patient’s current condition if certain criteria are met. Let’s examine them.
Criteria 1: “The documentation would need to substantiate that the services of skilled personnel are, in fact, required to achieve this goal.”
Key finding 1: You must document why a skilled therapist is needed to achieve the goal (maintain current condition).
Criteria 2: “Regularly documenting the degree to which the program’s treatment goals are being accomplished.”
Key finding 2: You must document the progress towards achieving the treatment goals regularly (i.e. more than once every ten visits).
Medicare clearly state’s in their LCD what the requirements are for a therapy visit to be covered. Here they are.
Therapy services are covered when they are rendered:
Medicare clearly states their requirements for developing a plan of care, which is required for any therapy visit to be covered:
Medicare provides guidelines for documentation for certain modalities. Here is an overview of the primary codes used in physical therapy. Over the next few weeks, we will provide more details on what is required for an initial evaluation, re-evaluation, and some of the lesser used CPT codes in physical therapy.
One of the core therapy treatment codes, 97110 requires the following documentation to support a billed unit. Medicare notes that often you will bill multiple units of 97110 on one claim.
Requirements:
Checks
Perform these checks when billing 97110
Medicare notes that this procedure is provided to improve balance, coordination, kinesthetic sense, posture, and proprioception and that the procedure may be reasonable and necessary for impairments that affect the body’s neuromuscular system. Some examples of this are poor static or dynamic sitting/standing balance, loss of gross and fine motor coordination, hypo/hypertonicity.
Checks:
There are multiple manual therapy techniques that Medicare will cover with proper documentation. Here is a breakdown of each technique and what is required.
Myofascial release/soft tissue mobilization
Medicare states that this treatment may be medically necessary for the treatment of restricted motion of soft tissues involving the extremities, trunk, or neck. Your documentation must clearly state the restriction and what specific techniques you provided. Some examples of techniques Medicare states are acceptable include the facilitation of fluid exchange, the restoration of movement in acutely edematous muscles, and stretching of shortened connective tissue.
Joint mobilization
Medicare states this can be medically necessary when the loss of articular motion and flexibility impedes the therapeutic procedure. You must clearly document the impairment and why joint mobilization is required.
Checks for manual therapy
Medicare will cover gait therapy for training patients whose walking abilities have been impaired by neurological, muscular, or skeletal abnormalities or trauma. Medicare will not cover this service if it is a repetitive walk-strengthening exercise for feeble/unstable patients or to increase endurance. Medicare will not cover gait therapy in conjunction with orthotic management and training unless the orthotic management and training was performed on an upper extremity.
Checks:
Medicare notes that this procedure involves using functional activities to improve functional performance. Some functional activities include bending, lifting, carrying, reaching, catching, and overhead activities. The activities should be targeted at a loss or restriction of mobility, strength, balance, or coordination.
Checks:
Medicare has determined that massage therapy may be necessary as adjunctive treatment to another therapeutic procedure on the same day. The therapy must be designed to restore muscle function, reduce edema, improve joint motion, or for relief of muscle spasm.
This is a common mistake therapists make when billing to Medicare (and United Healthcare).
Use G0283:
G0283 represents unattended electrical stimulation to one or more areas for indications other than wound care. Some of the possible treatments may include:
These treatments may be necessary during the initial phase of treatment if and only if there is an expectation of improvement in function or to prevent further deterioration.
G0283 is typically billed in conjunction with CPT code 97110. It is expected that G0283 is used in a clearly adjunctive role and not as a major component of the therapeutic encounter.
Checks for G0283:
Use CPT code 97032
CPT code 97032 also requires direct (one-on-one) patient contact by a qualified professional and clear documentation of the type of electrical stimulation provided, as well as the medical necessity of constant contact. Types of e-stim that might require constant contact include:
Billing 97032 requires supportive documentation at least every ten visits. The documentation required is:
Checks for 97032:
Prompt EMR was designed and developed with these documentation requirements in mind. Schedule a demo today to see the documentation features in action!
Help your practice grow
From intake to insights, Prompt is the all-in-one platform you need